Early Cancer Detection: Methods, Benefits, and Screening Options

By Dr. Letizia Gulino, PhD Head of Science & Technology, RMDM Group
Dr. Letizia Gulino is the Head of Science and Technology at RMDM Group, bringing over 20 years of extensive experience in molecular medicine research and private sector innovation. Holding a PhD in Molecular Medicine, Dr. Gulino has dedicated her career to advancing scientific understanding and developing cutting-edge solutions in health and disease. Her expertise bridges fundamental research and translational applications, making her a leading voice in the intersection of science, technology, and patient-centered innovation. At RMDM, she spearheads initiatives that integrate molecular insights with practical strategies to address complex diseases, reflecting her commitment to bridging science and real-world impact.
Introduction
In this article, we explore the various methods available today to identify cancer at an early, more treatable stage. We outline the significance of routine screening, examine the benefits of emerging technologies like liquid biopsy, and emphasise how innovative approaches can improve diagnostic accuracy. You’ll gain insights into both traditional and modern cancer screening tests, as well as the importance of patient education and proactive health management.
The Importance of Early Cancer Detection
Why Early Cancer Detection Matters
Early detection through an exam improves treatment success rates and better prognosis. Innovation in screening boosts cancer awareness while reducing disease burden and healthcare costs.
Awareness efforts, such as community initiatives, also aid in understanding lifestyle impacts and statistics linking early diagnosis to improved survival rates. These insights support a focused approach to cancer screening awareness.
Statistics on Cancer Survival Rates Linked to Early Detection
Robust statistical data demonstrates that early cancer detection significantly improves survival rates. The rise of early-onset cancer across younger demographics makes this even more critical. According to the American Cancer Society, the five-year relative survival rate for breast cancer detected at a localized stage is 99%, compared to 31% when diagnosed after metastasis (ACS, 2024).
Similarly, data from the National Cancer Institute’s SEER program shows that early-stage colorectal cancer has a 91% five-year survival rate, while late-stage detection drops this to just 15%.
Advanced diagnostic methods enable clinicians to identify cancer at its most treatable stage:
- Medical ultrasound – Non-invasive imaging for various cancer types
- Blood plasma analysis – Detects cancer markers in blood samples
- Multi-cancer blood-based tests – Screen for multiple cancer types simultaneously
Key Research Findings:
- Cohen et al. (2018): Multi-cancer blood testing detected 70+ cancer types with 99.3% specificity
- Mayo Clinic research: Combining imaging and molecular biomarkers improves detection accuracy for pancreatic and lung cancers
Clinical Benefits: Expert evaluations consistently highlight that verified screening programs play a central role in improving outcomes when implemented through licensed, quality-assured facilities. By relying on accredited technologies and evidence-based guidelines, health professionals can:
- Provide accurate, timely diagnoses
- Support better treatment decisions
- Build patient confidence in preventive strategies
Tools like PanTum Detect®, which detect metabolic activity of cancer cells responding to early-stage tumors, further expand the arsenal of effective, non-invasive early detection options, especially for asymptomatic individuals.
Public awareness of these statistics, paired with access to validated diagnostic tests, is essential to reducing mortality across cancer types.
KEY TAKEAWAY Early detection dramatically improves survival rates:
- Breast cancer: 99% survival when caught early vs 31% when late
- Colorectal cancer: 91% survival when caught early vs 15% when late Early intervention reduces treatment complexity and healthcare costs
Traditional Cancer Screening Methods
Mammograms for Breast Cancer Detection
Mammography remains the gold standard tool in breast cancer screening. This imaging technique captures detailed images of breast tissue to detect abnormalities, often before cancer symptoms appear. The ability to identify tumors at an early stage has made mammograms a key public health tool, especially in organised screening programs.
While mammography is highly effective, research continues into how blood-based biomarkers might augment imaging. Some studies, such as those published in JAMA, explore the potential of circulating tumor DNA (ctDNA) analysis as a complementary tool. However, it’s important to note that ctDNA detection depends on the shedding of genetic material by tumor cells into the bloodstream, something that may not occur in very early stages or with certain tumor types.
Colonoscopy for Colorectal Cancer Prevention
Colonoscopy remains a cornerstone in the early detection and prevention of colorectal cancer. As a direct visual examination of the colon and rectum, this procedure enables clinicians to identify tissue-level alterations, such as polyps, inflammation, or abnormal growth patterns, that may signal precancerous changes or malignancy. Unlike genetic mutations, which occur at the DNA level and are not visible through this method, colonoscopy focuses on the observable structural and morphological changes in the mucosal lining. Enhanced imaging and magnification further aid in distinguishing subtle tissue irregularities that might otherwise be overlooked.
Widely adopted in the United Kingdom and almost every other developed healthcare system, colonoscopy is recognised globally as a fundamental technique for colorectal cancer screening and risk reduction. Its proven effectiveness is often highlighted in public health campaigns and clinical outreach, emphasising its dual value: both as a diagnostic tool and a preventive intervention through polyp removal.
Numerous peer-reviewed publications support the clinical value of colonoscopy in reducing colorectal cancer incidence and mortality. For example, the landmark National Polyp Study (Winawer et al., 1993) demonstrated a significant reduction in colorectal cancer deaths through regular colonoscopic screening and polypectomy. More recent studies, such as the NordICC trial (Bretthauer et al., NEJM, 2022), continue to evaluate its population-wide impact in real-world settings.
Colonoscopy’s role is not just procedural, it represents a proactive step in cancer prevention, empowering both clinicians and patients with early, actionable information.
Pap Tests for Cervical Cancer Screening
Among the most impactful tools in early cancer detection, Pap tests have long stood as a key method for preventing cervical cancer. Often part of routine gynaecological exams, the Pap test involves collecting cells from the cervix to look for abnormal changes that could indicate a risk of cancer. These cellular changes, such as mild dysplasia or more severe lesions, can be identified well before symptoms appear, allowing for timely intervention and treatment.
Pap testing has proven highly effective when performed at regular intervals, significantly reducing the incidence and mortality associated with cervical cancer. In many countries, including those with national screening programs, Pap tests are often paired with HPV testing. This combined approach enhances the detection of high-risk strains of the human papillomavirus, which is known to be the leading cause of cervical cancer. International efforts, including WHO cervical cancer screening guidelines, continue to improve global access to cervical cancer prevention.
It’s important to clarify what the Pap test does and doesn’t do. It is a cytological examination that assesses the health of cervical cells. While other diagnostic methods, such as ultrasound or genetic testing, are used in women’s health to evaluate reproductive structures or hereditary cancer risk, the Pap test does not interpret or integrate data from these tools. Each test serves its own distinct role in a comprehensive diagnostic strategy.
Additionally, while hormonal changes can affect cervical cell appearance, the Pap test is not a tool for monitoring hormone levels or diagnosing hormone-related conditions. And contrary to occasional misunderstandings, Pap tests are not connected in any way to lung cancer screening, which relies on entirely different imaging techniques such as low-dose CT scans.
The enduring value of the Pap test lies in its simplicity, accessibility, and effectiveness. Ongoing research into less invasive cervical screening methods continues to improve patient experience while maintaining diagnostic accuracy. When combined with HPV screening and appropriate clinical follow-up, it offers a robust line of defence against one of the most preventable forms of cancer. Regular participation in cervical screening remains one of the most important steps individuals can take in managing their long-term health.
Advanced Imaging: MRI and CT Scans
Modern imaging technologies such as magnetic resonance imaging (MRI) and computed tomography (CT) scans are indispensable tools in the early detection and diagnosis of cancer. These high-resolution techniques allow clinicians to visualise internal organs and soft tissues in great detail, enabling the identification of tumors, lesions, or structural abnormalities that may indicate malignancy, often before symptoms arise.
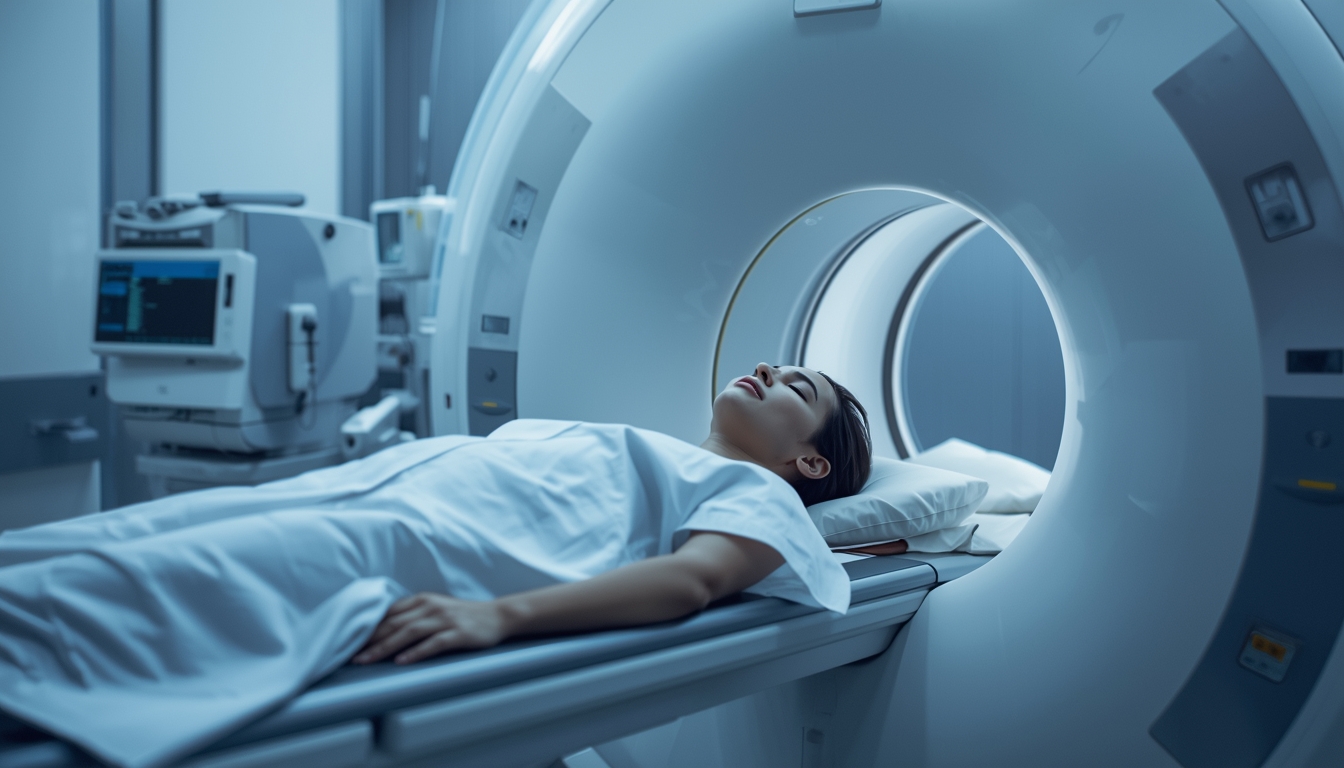
MRI and CT scans are widely used not only for diagnosis but also for treatment planning and monitoring disease progression. For example, MRI is especially valuable in detecting prostate, brain, and breast cancers, where soft-tissue contrast is crucial. Addressing prostate cancer screening challenges requires innovative approaches to improve early detection accuracy. [LG2] CT scans are routinely employed in screening for lung and colorectal cancers, as they can quickly capture images of large areas of the body with high spatial resolution.
Clinical evidence supports the critical role of these technologies in improving cancer outcomes. In lung cancer screening, the National Lung Screening Trial (Aberle et al., NEJM, 2011) demonstrated that low-dose CT scans reduced mortality by 20% in high-risk individuals compared to chest X-rays. Similarly, in colorectal cancer, CT colonography (Pickhardt et al., NEJM, 2003) has shown high sensitivity in detecting advanced adenomas and cancers, offering a less invasive alternative to traditional colonoscopy.
In breast cancer diagnostics, MRI screening (Kuhl et al., JCO, 2005) is recommended alongside mammography for high-risk individuals (e.g., BRCA mutation carriers), with studies showing increased detection rates of invasive cancers. The combination of imaging modalities allows for a more comprehensive view of potential pathology and reduces the likelihood of false negatives.
These advances are reflected in healthcare policy as well. Health insurance providers and national screening programs increasingly recognize the cost-effectiveness and clinical value of incorporating MRI and CT into routine screening for at-risk populations. This alignment between science and policy facilitates wider access to early diagnosis, which is essential in reducing cancer-related mortality and improving long-term patient outcomes.
KEY TAKEAWAY Established screening methods form the foundation of early detection:
- Mammograms: Gold standard for breast cancer screening
- Colonoscopy: Direct visualization prevents colorectal cancer
- Pap tests: Highly effective cervical cancer prevention
- Blood tests: Identify cancer markers before symptoms appear
Liquid Biopsy and Blood-Based Cancer Detection
The role of blood tests in identifying cancer markers plays a significant part in patient evaluation and treatment planning. Physicians use these tests to measure specific biomarkers that can signal abnormal cell changes, including specialized biomarkers in breast cancer research, which assist in making informed decisions about medication and further investigations. The method aligns with guidelines from the World Health Organisation, providing clear benefits in early detection and management strategies.
Expert evaluation of blood test results helps in tailoring individualised approaches for patients at various stages, including those undergoing menopause. By accurately measuring markers, physicians gain crucial insights that inform treatment plans, ensuring that patients receive appropriate medication and timely support. This approach has proven useful in clinical settings where early detection impacts long-term health outcomes.
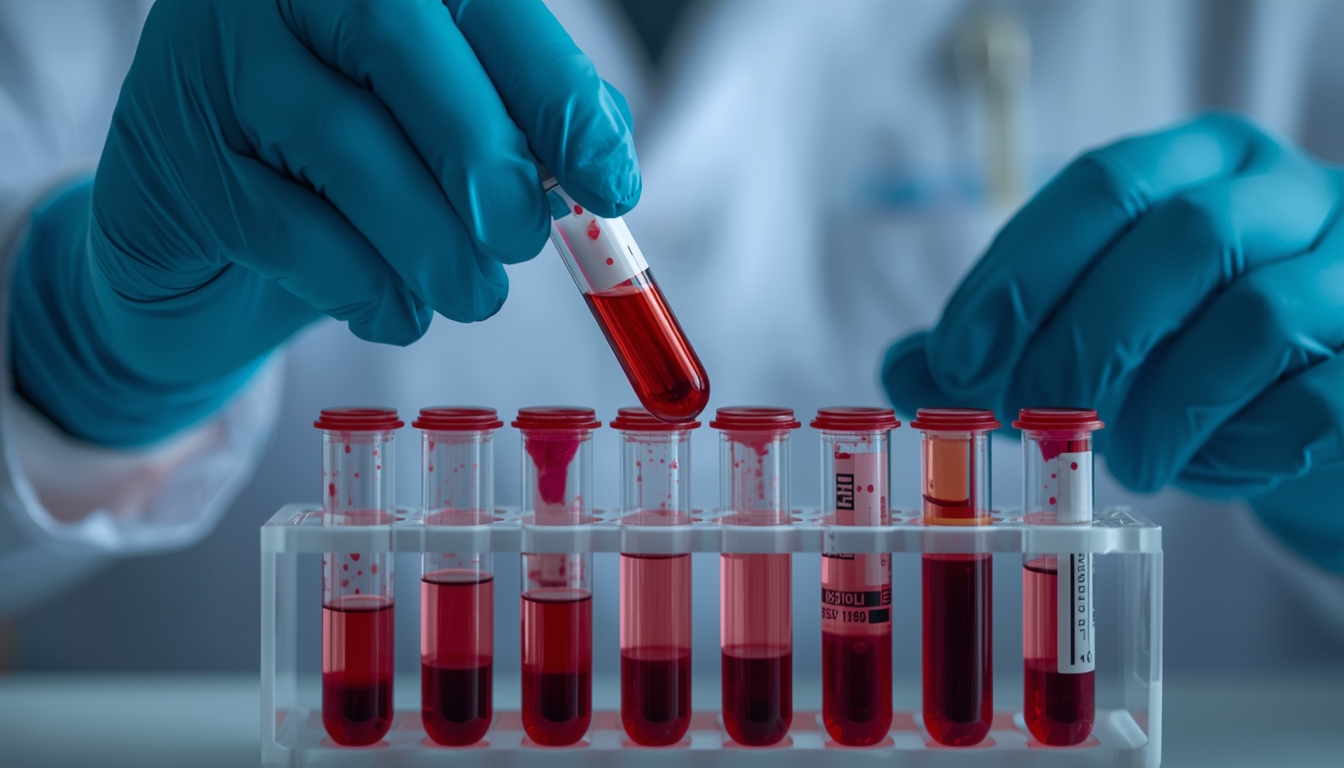
In routine clinical practice, the utilisation of blood tests supports ongoing evaluation and monitoring of patient health. Physicians rely on these tests as a tool to detect subtle changes in biological markers related to cancer, guiding their decisions on medication and treatment alterations. This process reflects the commitment of health professionals to improving diagnostic accuracy under the standards set by the World Health organization.
Emerging Technologies and the Future of Early Cancer Detection
Advanced Approaches Beyond Traditional Methods
Emerging technologies are transforming how clinicians approach early cancer detection, offering improved accuracy, broader applicability, and earlier intervention opportunities. Among the most impactful advances is DNA sequencing, which helps identify genetic mutations linked to various cancers, such as prostate, breast, and colorectal. By detecting these alterations at the molecular level, clinicians can stratify risk and adapt prevention or treatment strategies accordingly.
Alongside DNA-based diagnostics, novel approaches like liquid biopsies, which detect circulating tumor DNA (ctDNA), and methylation assays are gaining clinical attention. Advanced liquid biopsy technologies offer minimally invasive tools to assess tumor activity, especially in cancers that lack standardised screening programs. For example, recent studies (Liu et al., Annals of Oncology, 2020) show how methylation signatures in cell-free DNA can support the early detection of multiple cancer types with high specificity.
However, these approaches depend on the presence of tumour-derived material in the bloodstream—something that may be absent in very early stages or in slow-growing tumors.
PanTum Detect: A Revolutionary Approach
This is where PanTum Detect introduces a paradigm shift. Rather than relying on tumor cells or their DNA shedding into circulation, PanTum Detect identifies the body’s immune response to cancer. It detects tumour-associated antigens (TAAs) within monocytes, an earlier and potentially more consistent signal of malignant transformation.
This strategy allows PanTum Detect to:
- Operate independently of tumor size or shedding behaviour
- Detect a broad range of solid tumors, including those not covered by routine screening
- Flag malignant changes before visible structural alterations occur on imaging
By complementing traditional and genomic-based diagnostics, PanTum Detect broadens the reach of early detection. It’s a scalable, blood-based test that reflects a functional immune imprint of cancer, offering a new layer of insight in the early diagnosis landscape.
As emerging technologies evolve, the integration of immune-response-based tools like PanTum Detect with genomic, imaging, and cytological approaches will pave the way toward more inclusive and proactive screening programs, with the potential to catch cancers earlier and reduce mortality across populations.
Liquid Biopsy Innovation: Beyond ctDNA and CTCs
Emerging technologies are expanding the boundaries of early detection beyond ctDNA and circulating tumor cells (CTCs). One such innovation is PanTum Detect, a liquid biopsy test that takes a unique approach. Instead of detecting tumor material directly, this liquid biopsy analyzes the immune system’s response to cancer by identifying tumor-associated antigens within monocytes—an early signal of malignant transformation.
This methodology offers several key advantages:
- It does not rely on tumor cell shedding, which can be highly variable across cancer types and stages.
- It is potentially applicable to a wide range of cancers, including those with no established screening programs.
- It may detect malignancy before structural changes are visible on imaging, enabling earlier and potentially more effective intervention.
By detecting cancer-associated changes in immune cells, PanTum Detect opens a new path in population-wide cancer screening: one that is proactive, minimally invasive, and scalable.
🔬 Learn About PanTum Detect Technology Discover the science behind this innovative approach to early cancer detection. Learn More About the Technology →
KEY TAKEAWAY Next-generation detection goes beyond traditional methods:
- PanTum Detect identifies immune response to cancer
- Works independently of tumor size or shedding
- Detects broad range of solid tumors before visible changes
- Complements existing screening programs
The Personal Benefits of Early Cancer Detection
How Early Detection Improves Treatment Success Rates
Detecting cancer at an early stage enables healthcare professionals to intervene promptly, often before the disease advances or spreads. This early intervention enhances the effectiveness of multiple treatment approaches:
- Surgery – More precise, less invasive procedures when tumors are smaller
- Radiation therapy – More targeted treatment with fewer side effects
- Adjuvant therapies – Additional treatments to reduce recurrence risk after tumor removal
Numerous studies confirm that early diagnosis improves survival rates and quality of life by allowing more precise, tailored treatment plans. Research consistently shows the positive correlation between early detection and patient outcomes.
Clinical Evidence: For example, timely detection of colorectal cancer through stool-based screening tests, such as the faecal immunochemical test (FIT) or stool DNA assays, provides clinicians with actionable information to recommend appropriate follow-up procedures like colonoscopy or surgery (Imperiale et al., NEJM, 2014).
Advanced Treatment Benefits: Early identification of abnormal cellular changes also supports the use of targeted therapies—drugs designed to attack specific cancer mutations or pathways—combined with ongoing monitoring through imaging or blood-based biomarkers. This integrated approach facilitates personalised care that adapts to individual patient responses, improving outcomes and minimising unnecessary treatments.
Moreover, early detection allows for strategic tissue sampling and molecular profiling, which help oncologists select optimal therapies and refine treatment plans as new evidence emerges. The ongoing accumulation of clinical data from early-stage cancers is critical in advancing adjuvant therapies and improving long-term survival.
Healthcare System Benefits: By investing in and adhering to evidence-based screening and diagnostic protocols, healthcare systems can maximise treatment success rates, reduce the burden of advanced disease, and ultimately save lives.
The Psychological Benefits of Peace of Mind From Early Tests
Early tests provide significant reassurance, as individuals gain clarity on their health status and reduce uncertainty about potential cancer risk factors. This clear information plays a vital role in hospital settings where doctors integrate findings from epigenetics studies, ensuring tailored interventions and reducing anxiety among patients.

Regular screening and early testing support mental well-being, as they help clarify whether common symptoms like diarrhea are linked to underlying conditions. Such diagnostic processes, often guided by data from public health authorities, offer individuals a proactive stance in managing their overall health.
The accessibility of early detection methods enhances public confidence and enables patients to address risk factors effectively. Health professionals in hospital environments utilise comprehensive testing that includes insights from epigenetics and clinical evaluations, providing peace of mind and reducing stress over unverified symptoms.
Potential Quality-of-Life Improvements Through Early Diagnosis
Early diagnosis improves quality of life by enabling targeted treatments that minimise potential side effects and maximise treatment success. Access to rapid results from liquid biopsy tests like PanTum Detect helps streamline decisions that influence the treatment pathway, thereby reducing the incidence of complications. Patients are encouraged to contact health professionals for guidance on the latest diagnostic tools and personalised advice.
Timely identification of genetic markers for example, like BRCA1, informs clinicians in their pursuit of a cure, ensuring that interventions are both effective and efficient. Professionals provide clear, actionable insights from diagnostic outcomes that help reduce uncertainty, thus bolstering patient confidence during the treatment process. This approach translates into marked improvements in overall well-being and day-to-day functionality.
Enhanced quality of life becomes an attainable goal when early detection techniques facilitate customised care plans tailored to individual needs. The integration of advanced methods, including liquid biopsy, supports a proactive stance against rising incidence rates, offering reassurance on the path towards a cure. Stakeholders are urged to exchange information via email to stay informed on the benefits of early detection and ongoing research breakthroughs.
The Role of Early Detection in Reducing Healthcare Costs
Early cancer detection significantly reduces healthcare costs by enabling interventions when symptoms and complications are less severe. The costs of late-stage cancer diagnosis are substantially higher than early intervention. This often results in less extensive and less expensive treatment regimens, improving both patient outcomes and the efficiency of care delivery.
Ongoing research, including important studies conducted in California, continues to demonstrate that early diagnosis supports more cost-effective approaches to cancer management and treatment.
Detecting cancer at an earlier stage frequently leads to shorter hospital stays, reduced need for aggressive therapies, and lower reliance on costly medications.
Timely identification of cancer provides healthcare professionals with actionable information that enhances patient management while mitigating additional medical expenses associated with advanced disease. Healthcare systems worldwide face challenges with cancer diagnosis backlogs, making early detection even more critical for system efficiency. Integrating early detection into routine care not only improves clinical outcomes but also facilitates the ongoing evaluation and refinement of diagnostic and treatment protocols, ultimately contributing to sustainable cost reductions across healthcare systems.
KEY TAKEAWAY Early detection benefits extend beyond individual health:
- Reduces treatment side effects and improves quality of life
- Significantly lowers healthcare system costs
- Provides peace of mind and reduces anxiety
- Supports family and community health outcomes
The Role of Technology in Cancer Detection Methods
AI-Powered Medical Imaging
Technology is changing the way we detect cancer, making it faster, more accurate, and more accessible than ever before. Today, doctors are using powerful cancer detection technology like 3D mammograms, low-dose CT scans, and even artificial intelligence (AI) to spot signs of cancer earlier, often before symptoms appear.
One example is low-dose CT scans, now used to screen people at high risk for lung cancer. This method can detect very small tumors that traditional X-rays often miss, helping doctors catch cancer early when it’s easier to treat. Another innovation, 3D mammography (also called tomosynthesis), creates detailed breast images that help reduce unnecessary biopsies and give clearer answers during routine screenings.
Technology is also making cancer detection smarter. New AI programs can analyse medical images and sometimes spot things that even trained eyes might overlook. For instance, in recent studies, AI has helped radiologists improve accuracy when reading breast scans, leading to fewer missed cases and fewer false alarms.

These tools aren’t just found in big hospitals anymore. Mobile screening units, digital platforms, and telemedicine services are helping bring early detection to more people, including those in rural or underserved communities. The need for accessible cancer detection in developing countries highlights the importance of scalable, cost-effective technologies. This means that where you live no longer has to determine how soon you get help.
Thanks to these advances, doctors can better monitor changes in the body over time and act quickly. Whether it’s through a scan, a blood test, or an AI-powered image review, technology is helping detect cancer at its earliest and most treatable stages, offering patients the best possible chance for a healthier future.
Machine Learning in Cancer Diagnosis
Machine learning is transforming cancer diagnosis by helping doctors detect early signs of disease with greater accuracy. These algorithms can quickly analyse complex medical data, such as test results, scans, and physical exam findings, to identify patterns that may signal the presence of cancer, often before symptoms appear.
One key advantage is their ability to reduce human error. By automating parts of the diagnostic process, especially in image analysis, machine learning helps doctors spot subtle changes in tissues or biomarkers that might otherwise be missed. Recent studies, reviewed by medical experts, confirm that these tools can significantly improve the reliability of early cancer detection.
A real-world example comes from Google Health, which developed an AI system that reads mammograms. In one large study, the system outperformed radiologists in detecting breast cancer, reducing false positives and missed diagnoses. This kind of innovation shows how machine learning can actively support medical teams in delivering faster, more accurate results.
Machine learning also speeds up diagnosis by sorting through large volumes of patient information to deliver clear insights. It can identify inflammation or unusual biological markers that are important in catching cancer early. Experts agree that integrating these tools into diagnostics supports timely decisions, earlier treatment, and better outcomes.
As research continues to validate their effectiveness, machine learning algorithms are becoming a trusted part of modern cancer care, offering both patients and clinicians a smarter, more confident way to manage health.
Cancer Detection Mobile Applications
Mobile applications are increasingly being developed to support cancer screening and early detection efforts, though they serve as supplementary tools rather than replacements for professional medical screening.
Some mobile health applications include features for cancer risk assessment questionnaires, screening appointment reminders based on age and risk factors, and educational content about cancer warning signs. Certain apps provide guidance for self-examinations, such as breast self-examination instructions, while others focus on tracking symptoms or changes over time.
These applications complement professional medical screening by helping users maintain awareness of recommended screening schedules, document health observations, and access educational resources about early detection. However, it’s important to note that mobile apps are not diagnostic tools and cannot replace professional medical evaluation for cancer detection.
Remote Cancer Screening and Consultation
Telemedicine is expanding access to cancer screening services and early detection consultations, particularly for individuals in underserved or remote areas where specialist access may be limited.
Remote screening services include virtual consultations for cancer risk assessment, telehealth appointments to discuss screening schedules and family history, and remote review of screening results with specialists. These services help ensure that geographic barriers don’t prevent timely cancer screening recommendations.
Additionally, telemedicine enables remote interpretation of certain diagnostic tests, including preliminary review of imaging and liquid biopsy results with specialists. This approach can reduce delays between testing and specialist consultation, supporting faster decision-making about follow-up care when screening results indicate potential concerns.
While telemedicine cannot replace hands-on screening procedures like colonoscopies or mammograms, it serves as an important bridge in the early detection process, ensuring patients receive timely access to specialist expertise for screening guidance and result interpretation.
Genetic Testing Innovations
Recent innovations in genetic testing have transformed how clinicians assess inherited cancer risk through the identification of mutations in key genes.
Key genes :
- BRCA1 and BRCA2 – Linked to breast and ovarian cancer risk
- MLH1 and MSH2 – Associated with Lynch syndrome and higher risk of colorectal/endometrial cancers
- Melanoma-related genes – Hereditary (familial): CDKN2A, CDK4, BAP1, MITF, TP53, Identify inherited skin cancer predisposition.
- Somatic (in the tumor): BRAF, NRAS, KIT, NF1, PTEN, TERT
- Inherited pancreatic cancer risk – Detected through genetic testing (e.g. BRCA1/2, PALB2, CDKN2A)
- Prostate cancer variants: assessing inherited susceptibility
Personalized Intervention Options:
- Enhanced surveillance – More frequent screening for high-risk individuals
- Preventive treatments – Proactive medical interventions to reduce risk
- Lifestyle modifications – Targeted changes based on genetic profile
- Family planning guidance – Informed decisions about hereditary risk
- Multi-gene panel testing – Comprehensive analysis for broader risk assessment
Environmental Risk Integration: Beyond cancer, innovations in whole-exome and genome sequencing reveal how certain genetic variants interact with environmental exposures, like smoking or chronic inflammation, to elevate cancer risk. These insights help doctors recommend targeted screening strategies, such as earlier colonoscopies for Lynch syndrome or annual skin checks for those with melanoma-prone gene mutations.
Real-World Testing Programs: Real-world examples include programs like Myriad myRisk, Color Genomics, or Invitae, which offer accessible genetic testing with detailed risk reports. Combined with genetic counseling, these services are helping more people make informed decisions about their care, even before symptoms appear.
As genetic testing continues to evolve, its role in cancer prevention will only grow stronger, empowering patients and physicians to act before cancer develops.
The Future of AI in Detection
Artificial intelligence software in early cancer detection represents a significant advancement, offering precise analysis of diagnostic images to identify signs of metastasis in critical areas such as the bone and brain. This approach provides clarity in identifying early changes, thereby fostering a more reliable screening process.
Experts note that AI-enhanced software aids in processing extensive datasets, which streamlines the detection of cells that could indicate early metastasis. The technology supports health care teams in optimising informed consent procedures by clearly explaining the benefits and risks associated with novel diagnostic methods.
Practical applications of AI have been demonstrated in clinical practices, where sophisticated software analyses contribute to a more efficient diagnostic workflow. These improvements facilitate earlier interventions that are particularly beneficial in monitoring sensitive regions like the bone and brain, ensuring that patients receive timely care.
Cancer Screening Awareness and Early Diagnosis
How Awareness Drives Early Detection
Awareness plays a critical role in the early diagnosis of cancer. When individuals understand the importance of regular health monitoring, such as an annual blood test, they are more likely to participate in preventive care that can identify disease in its earliest, most treatable stages. Public advocacy efforts, including calls for prostate cancer testing reform, demonstrate the growing demand for improved screening access. Clear guidelines and public health initiatives around screening programs further enhance awareness and encourage proactive action.
A key example of this approach is the PanTum Detect® blood test, which is designed to act as an annual screening tool for healthy, symptom-free individuals. Unlike traditional diagnostic methods that rely on the detection of tumor material, PanTum Detect® identifies immune responses triggered by cancer at a very early stage. By combining the test with targeted imaging, this method supports earlier diagnosis and reduces the risk of late-stage discovery.
Clinical data on sensitivity and specificity supports the reliability of such screening strategies in detecting subtle biological changes before symptoms arise. When paired with public education, these tools can significantly shorten diagnostic timelines and improve treatment outcomes.
By increasing public access to accurate information and encouraging the use of innovative diagnostics like PanTum Detect®, healthcare providers can support timely interventions, better disease management, and a meaningful reduction in cancer-related mortality.
The Influence of Lifestyle Changes on Early Detection Outcomes
While lifestyle choices do not directly improve the accuracy of diagnostic tools, they play a crucial role in shaping how and when individuals access screening. For instance, people who follow preventive health routines, such as exercising, not smoking, and attending regular medical check-ups, are significantly more likely to undergo early cancer screening (ACS, 2023). Comprehensive cancer prevention strategies encompass both lifestyle modifications and regular screening protocols.
Studies have shown that smoking cessation improves the performance of low-dose CT scans for lung cancer screening, while maintaining a healthy weight can reduce imaging artifacts in mammography and abdominal ultrasounds (NCI, 2021). Understanding the relationship between cancer and nutrition provides additional insights into prevention strategies. These lifestyle factors indirectly enhance early detection outcomes by ensuring higher-quality imaging and more consistent screening adherence.
Moreover, public health campaigns linking healthy behaviours with cancer awareness have led to increased participation in colorectal and cervical screening programs, underscoring the link between lifestyle and timely diagnosis.
Community Initiatives Focused on Cancer Screening Awareness
Community Screening Initiative Benefits:
- Facilitate early diagnosis – Programs focus on identifying cancer before symptoms appear
- Improve medical practices – Promote standardized, evidence-based screening procedures
- Follow established guidelines – Adhere to CDC and clinical laboratory improvement standards
- Provide practical pathways – Give individuals clear steps to address health concerns
- Achieve better outcomes – Enable more effective community-wide health management
Professional Education & Outreach: Health professionals also use community programmes to educate the public on early diagnosis techniques and the importance of timely screening. Programs supported by recognised agencies offer comprehensive information on diagnostic procedures, creating a bridge between clinical research and everyday medicine. This connection empowers communities with validated data, ensuring that residents make informed decisions based on current health guidelines.
Local Implementation Success: Local efforts to enhance screening awareness have led to practical improvements in service delivery, fostering trust between health institutions and the public. By integrating reliable credentials and evidence from centres for disease control and prevention, these initiatives support clear diagnosis pathways and regular screening intervals. This synergy between community action and formal medicine practice offers a robust approach to managing public health challenges effectively.
Public Health Campaigns Aimed at Early Detection Awareness
Public health campaigns aimed at promoting early detection have become an essential pillar of preventive medicine, leading to measurable improvements in community awareness and health-seeking behaviour. These initiatives are particularly impactful in addressing conditions like ovarian cancer, where early-stage symptoms are often vague and easily overlooked. Through evidence-based messaging, often supported by peer-reviewed research such as that published in The BMJ, these campaigns translate complex clinical data, such as findings from radiology and biomarker studies, into accessible, actionable knowledge for the public.
Effective campaigns go beyond simply raising awareness; they empower individuals with practical steps to recognise early warning signs, navigate healthcare systems, and seek timely diagnostic evaluations. For example, the UK’s Be Clear on Cancer campaign and Australia’s Find Cancer Early initiative have demonstrated increased rates of early clinical presentation and improved cancer staging at diagnosis. These efforts often combine mass media outreach with community-based education, ensuring the message reaches diverse populations.
Furthermore, successful campaigns integrate multidisciplinary collaboration: oncologists, radiologists, general practitioners, and public health experts work alongside community leaders to tailor messaging to cultural and demographic needs. Visual tools such as ultrasound images and symptom checklists are used to demystify medical concepts and foster trust. While lifestyle elements like exercise and nutrition are included, they serve as complementary messages to the primary goal of symptom awareness and early clinical engagement.
Crucially, the impact of these campaigns is supported by data. Studies have shown a correlation between campaign exposure and increased screening uptake, particularly in populations previously underrepresented in preventive care. Public health campaigns thus serve not only as educational tools but as catalysts for system-wide improvement in early detection and survival outcomes.
Cancer Screening Programs and Follow-Up Care
How Regular Screenings Can Lead to Earlier Interventions
Regular screenings offer a structured approach that helps identify potential health concerns before symptoms arise, allowing for earlier and more effective early intervention strategies. In clinical practice, particularly in countries like the United States, routine cancer screening is increasingly supported by centralised databases that promote consistent monitoring and uphold strong ethical standards in healthcare decision-making.
PanTum Detect® plays a key role in this context. As a multi-tumor blood screening test designed for healthy, asymptomatic individuals, it is recommended once a year as part of a regular health check-up. If the test result is near the positivity threshold, a follow-up test after six months can help clarify the situation. In cases of a positive PanTum Detect® result, medical guidelines suggest proceeding with diagnostic imaging to investigate possible tumor activity more closely.
The integration of routine screenings with tools like PanTum Detect®, supported by comprehensive databases, ensures that clinicians can access reliable data to tailor early interventions. This approach not only reduces diagnostic uncertainty but also enables more precise and timely care, highlighting the growing importance of early detection strategies in modern healthcare.
Creating Your Personal Screening Schedule
Step-by-Step Guide to Creating Your Personal Screening Schedule:
Step 1: Assess Your Cancer Risk Factors
- Family history – Document any cancer cases in immediate and extended family
- Personal health history – Review previous test results and medical conditions
- Lifestyle factors – Consider smoking, diet, exercise, and environmental exposures
- Genetic factors – Discuss potential hereditary cancer syndromes with your provider
Step 2: Consult Healthcare Professionals
- Primary care physician – Start with comprehensive health assessment
- Specialists and oncologists – Get referrals to cancer specialists or genetic counselors if needed
- Multiple opinions – Consider second opinions for complex risk assessments
Step 3: Choose Appropriate Screening Methods
- Standard screenings – Annual mammograms, colonoscopies, Pap tests as recommended
- Blood-based tests – Consider multi-cancer detection tests for broader coverage
- Advanced imaging – MRI or CT scans for high-risk individuals
- Genetic testing – DNA analysis for inherited cancer predisposition
Step 4: Establish Testing Timeline
- Annual screenings – Most cancer detection tests recommended yearly
- Age-based milestones – Follow guidelines for when to start specific screenings
- Risk-adjusted frequency – More frequent testing for high-risk individuals
- Regular follow-ups – Schedule consistent monitoring to track any changes
Step 5: Monitor and Adjust
- Track results – Keep detailed records of all screening outcomes
- Review annually – Reassess risk factors and screening needs with your provider
- Stay informed – Keep up with new screening technologies and recommendations
- Prompt follow-up – Address any concerning results immediately
Follow-Up Tests After Screenings
Following initial screening tests, follow-up examinations are essential for confirming results and informing subsequent clinical decisions. Medical specialists—particularly oncologists and diagnostic experts, emphasise that additional testing, including biomarker analysis or imaging, provides the critical depth needed for accurate diagnosis and tailored treatment strategies. The role of blood testing after cancer surgery extends monitoring beyond initial detection to ongoing care management. Timely follow-up tests serve not only to validate initial findings but also to clarify any uncertainties, enhancing the precision of care.
Experts often highlight in public forums such as podcasts how this practice supports transparent, data-driven decision-making and strengthens early cancer detection protocols. By committing to further investigation, healthcare teams can adapt screening pathways in real time, offering patients a proactive and evidence-based approach to managing potential risks.
Accessing Cancer Screening Services
Successfully participating in cancer screening requires both practical preparation and addressing common barriers that may prevent individuals from seeking timely care.
Overcoming Common Screening Barriers:
- Education and preparation – Understanding what screening tests involve and their benefits in early detection
- Clear communication – Asking healthcare providers specific questions about procedures and results
- Scheduling strategies – Creating structured, personalized screening schedules based on individual risk factors
- Anxiety management – Focusing on screening as proactive health control rather than fearful obligation
- Support systems – Utilizing healthcare staff guidance and support throughout the screening process
Regular screening participation improves when individuals view tests as valuable health investments rather than isolated medical events. Healthcare providers emphasize that understanding the early detection benefits and maintaining open communication about concerns leads to better screening adherence and ultimately better health outcomes.
The Value of Support Groups in Cancer Care
Support groups play a vital role in helping patients navigate the emotional and practical challenges of cancer care. By creating a space for individuals to share experiences, these groups foster mutual encouragement and provide strategies that have been shown to improve both quality of life and adherence to care plans, factors that can positively influence survival outcomes.
In professionally facilitated groups, patients often find reassurance through open discussions about their concerns, including anxiety around screenings, diagnostic procedures, and life transitions such as pregnancy. These conversations help demystify the clinical process and make it easier for individuals to follow recommended follow-up care and make informed decisions.

Through peer connection and expert input, patients become better equipped to understand their medical journey, interpret results, and recognise early warning signs, empowering them to take timely, proactive steps. With advancements in diagnostic technology supporting earlier detection, support groups serve as a bridge between clinical care and emotional resilience, reinforcing the importance of community in long-term cancer management.
Patient Advocacy and Education in Cancer Detection
How Patients Can Advocate for Their Health:
- Research diagnostic technologies – Learn about advanced tests
- Consult specialized experts – Seek guidance from leading cancer centers globally
- Understand all options – Get clear information about various diagnostic methods
- Balance risk and benefit – Make informed decisions tailored to your circumstances
- Ask specific questions – Inquire about the relevance and utility of different tests
Building Healthcare Partnerships: Emphasising patient advocacy encourages direct engagement with specialised clinics and cancer centres worldwide, where health professionals provide actionable insights into the progression of cancer markers like circulating tumor cells. Clear communication about the advantages of early detection methods helps patients understand what to expect from the diagnostic process and how timely detection can contribute to personalised care plans.
Global Expertise Access: Expert advice from renowned centres globally reinforces awareness of the critical balance between early detection benefits and overall treatment outcomes. This empowered stance promotes open communication between patients and healthcare providers, ensuring a more informed, guided, and effective cancer detection journey regardless of geographic location.
The Significance of Patient Education on Screening Options
Patient education on screening options plays a critical role in ensuring individuals understand the benefits of early detection and available diagnostic technologies.
Key Education Components for Patient Screening Awareness:
- Diagnostic Technology Awareness:
Understand the purpose and benefits of tools like MRI, CT scans, and liquid biopsies in early detection. - Screening Literacy:
Learn how test types and screening frequency affect early diagnosis and health outcomes. - Biomarker Understanding:
Know how blood tests and other tools detect cancer-related markers with high precision. - Insurance Navigation:
Understand coverage rules and authorization steps to access suitable screening tests. - Preventive Strategies:
Recognize the role of vaccines and other measures in reducing disease risk. - Healthcare System Navigation:
Learn how to access, schedule, and prioritize diagnostic services confidently.
Patient Empowerment Benefits:
- Informed decision-making – Choose screening methods tailored to individual needs
- Confident healthcare navigation – Engage effectively with providers and systems
- Proactive health management – Take charge of personal screening schedules
- Better provider relationships – Engage meaningfully with healthcare teams
- Improved outcomes – Make choices that support long-term health goals
The Result: Experts consistently show that informed patients are better equipped to engage with healthcare providers and select screening methods that support improved long-term outcomes.
Resources for Staying Informed About Cancer Detection Trends
Staying updated on cancer detection trends is essential for informed decision-making. Peer-reviewed journals and clinical trial reports offer transparent, evidence-based insights into evolving screening methods. By following reputable open-access platforms, both patients and professionals can track the latest developments in early detection and align with best practices in preventive care.
How to Navigate Health Systems for Better Access to Care
Navigating today’s healthcare systems can be overwhelming, but understanding key resources and strategies can significantly improve your access to timely care.
Essential Healthcare Navigation Tools:
- Online patient portals – Access test results, schedule appointments, and communicate with providers
- Referral systems – Understand the process for getting specialist consultations
- Community health navigators – Utilize local support services for guidance
- Insurance resources – Know your coverage and authorization requirements
Key Support Personnel to Engage:
- Healthcare advocates – Help clarify complex processes and procedures
- Case managers – Coordinate care between multiple providers
- Support staff – Assist with appointment scheduling and insurance issues
- Patient representatives – Address concerns and resolve system barriers
Action Steps for Better Access:
- Learn the system – Understand your healthcare network’s specific processes
- Know who to contact – Keep key phone numbers and contacts readily available
- Understand required forms – Know what paperwork is needed in advance
- Follow up consistently – Don’t wait for others to call you back
- Ask questions – Request clarification when processes aren’t clear
Taking control of your health journey with these strategies helps ensure that no time is lost in receiving appropriate care, particularly for time-sensitive early detection services.
The Influence of Support Networks on Cancer Care Choices
Support networks play a pivotal role in shaping cancer care decisions by offering patients clear guidance, shared experiences, and access to trusted information. Whether navigating breast or colorectal cancer screenings, individuals benefit from discussions that highlight the importance of early detection and regular check-ups as tools for preserving long-term health.
These networks also play a critical role in educating patients about their rights, such as how to submit a request for access to protected health information. This understanding empowers individuals to participate actively in their health management and ensures that they remain informed about diagnostic developments and care options.
By combining practical advice with real-world perspectives, support networks simplify complex topics like screening protocols and risk factors.
The Future of Early Cancer Detection: An Integrated Approach
Building Comprehensive Detection Programs
As healthcare shifts toward precision and prevention, combining traditional and molecular diagnostics will likely become the standard. Mammograms, colonoscopies, and other routine screenings remain essential, but tools like PanTum Detect® offer the opportunity to broaden early detection coverage and catch cancers that would otherwise go unnoticed.
Investing in education, accessibility, and further research will be crucial to fully realising the benefits of these innovations. Early detection not only improves survival rates but it also reduces treatment burdens, healthcare costs, and patient anxiety.
Conclusion
Early detection methods provide clear advantages in identifying cancer at a stage where treatments can be more effective. They offer actionable insights that support healthcare professionals in crafting individualised care plans. Proactive screening improves patient outcomes, contributes to cost-effective healthcare, and reduces uncertainty for patients. This approach strengthens public confidence, reinforces community wellness, and fosters a lasting commitment to early diagnosis and treatment.
Medical Review: This article has been authored and reviewed by Dr. Letizia Gulino, PhD, molecular biologist specializing in oncology research. Last reviewed: 1st August 2025. The information is for educational purposes and should complement, not replace, professional medical consultation.
Frequently Asked Questions
1. What are the latest advancements in early cancer detection methods?
Recent advancements in cancer screening provide an earlier, more accurate detection using a mix of molecular, imaging, and computational technologies.
Blood-based liquid biopsies detect circulating tumor DNA, RNA proteins and markers.
Non-blood tests that analyse saliva, urine, stool or breath for tumor- associated biomarkers.
Advanced imaging like fluorescence or Raman spectroscopy, enable precise visualization of tumors at early stages.
AI integrates imaging, molecular tests, and clinical data to detect subtle patterns, improving diagnostic accuracy and supporting earlier intervention.
These advancements enable detection of multiple cancer types from single tests with high specificity, often before symptoms appear.
2. What is liquid biopsy cancer screening?
Liquid biopsy cancer screening is a method that analyses a patient’s blood to detect cancer-related biomarkers, such as circulating tumour DNA , circulating tumour cells , tumour-derived proteins, or other biomarkers. Unlike traditional tissue biopsies, which require surgical sampling of tumour tissue, liquid biopsies are minimally invasive and require only a blood draw. Certain platforms aim to detect multiple cancer types from a single sample, potentially enabling earlier diagnosis, sometimes even before symptoms appear.
PanTum Detect is an example of this technology, which identifying immune system responses to cancer. Learn more about PanTum Detect →
3. Can AI assist in identifying cancer biomarkers?
AI plays a crucial role in modern cancer biomarker research and identification.
How AI helps identify biomarkers:
- Analyzes large-scale datasets – Processes genomic, proteomic, imaging and clinical data from various cancer types
- Pattern recognition – Identifies subtle correlations between biomarker profiles and cancer risk
- Rapid processing – Automatically detects potential biomarker candidates much faster than traditional methods
- Similarity-based comparisons Compares patterns across different patient groups
Key advantages:
Speed and accuracy – AI can process vast amounts of data quickly and precisely
Discovery of new biomarkers – Identifies previously unknown biomarker combinations
Personalized medicine – Helps develop targeted biomarker panels for individual patients
Continuous learning – AI systems improve as more data becomes available
AI is revolutionizing biomarker discovery, making it faster and more accurate than ever before.
4. How does genetic testing detect cancer?
Genetic testing can help detect cancer or assess cancer risk by identifying specific genetic mutations and in some cases, changes in gene expression associated with cancer development. These alterations can often be detected in blood or tissue samples before symptoms appear. Recent advances including AI integration and large genomic databases have made genetic testing more accurate and accessible. This enables earlier diagnosis and more effective treatment by spotting cancer-related DNA changes at the molecular level.
5. How effective are blood tests for cancer screening?
Blood tests for cancer screening are becoming highly effective due to advances in liquid biopsy and multi-cancer early detection technologies. These tests analyse circulating tumor DNA, cell-free DNA, and specific biomarkers to detect multiple cancer types non-invasively They offer high specificity and good sensitivity, making them especially valuable for cancers lacking established screening methods. Tests like PanTum Detect represent this new generation of screening technology.
6. What are the benefits of medical imaging for cancer detection?
Medical imaging for cancer screening offers several key advantages: it’s non-invasive and safer than surgical procedures, can detect tumors also before symptoms appear, provides precise information about tumor size and location, and allows doctors to monitor treatment progress over time. Imaging techniques like CT, MRI, and mammography have become essential tools for early cancer detection and ongoing patient care.
7. Can cancer vaccines help in early detection?
No, cancer vaccines do not help with early detection. Cancer vaccines are tools designed to prevent or treat cancer, not detect it. Examples : Vaccines for HPV, which prevent virus-related cancers by targeting the infectious agent or therapeutic vaccines which are designed to stimulate the immune system to fight existing cancer. Neither type plays a role in cancer detection or screening.
8. Can MRI scans find cancer?
Yes, MRI scans can help detect cancer by using powerful magnetic fields and radio waves to create detailed images. cancerous tissues indeed behave differently than normal tissues due to variations in water content and cell density. This creates clear contrasts on images that help radiologists identify tumors. Contrast agents can be injected to make tumors even more visible, and advanced MRI techniques provide additional details about tumor characteristics and blood supply.
9. Why are tumor markers important for cancer detection?
Tumor markers are extremely important in cancer detection because they provide early warning signs and help guide treatment decisions. They are proteins made by cancer cells or by the body in response to cancer, and can be found in blood, urine, or tissue. Testing for tumor markers can help indicate whether cancer might be present, how advanced it is, or how well treatment is working. Tumor markers alone cannot confirm cancer, but they are among the first steps of analysis to guide doctors in deciding if further tests are needed to define a final diagnosis.
10. Can urine tests detect bladder cancer early?
Urine tests can detect signs like blood in the urine, which may suggest a problem such as bladder cancer. However, they are not reliable enough on their own to diagnose or screen for bladder cancer. For a confirmed diagnosis, more accurate methods like cystoscopy are needed.
11. How does AI improve cancer diagnosis?
AI can assist physicians in cancer diagnosis by rapidly analyzing medical images and other diagnostic data to highlight patterns or suspicious areas that may require closer examination. While AI can help detect subtle signs that might be overlooked, it does not replace the doctor’s judgment. The final diagnosis and treatment decisions are always made by medical professionals, with AI serving as a supportive tool.
12. How early can cancer be detected?
Cancer can potentially be detected through cancer screening months or even years before symptoms appear, depending on the cancer type and screening method used. Liquid biopsy tests may detect cancer 6-18 months before symptoms, while imaging screening can detect tumors 1-3 years before they become noticeable. The earlier cancer is detected, the higher the survival rates and the less invasive the treatment required.
13. What is the most accurate cancer screening test?
There is no single “most accurate” cancer screening test because each test is designed for different cancer types and works best in certain contexts. For example, Colonoscopy achieves over 90% accuracy for colorectal cancer, while mammography combined with MRI reaches up to 95% accuracy for breast cancer in high-risk individuals. The most effective approach is using multiple screening methods appropriate for yourindividual risk profile rather than relying on any single test.
14. What are the signs of early stage cancer?
Early stage cancer often produces no symptoms at all, which is why regular screening is crucial. When symptoms do occur, they may include unexplained weight loss, persistent fatigue, unusual bleeding, changes in skin or moles, persistent pain, or changes in bathroom habits. However, these signs can have many non-cancerous causes, so any persistent symptoms lasting more than 2-3 weeks should be evaluated by a healthcare provider.
15. Can cancer be detected before symptoms appear?
Yes, some cancers can often be detected before symptoms appear through routine screening tests like mammograms, colonoscopies, and Pap tests, as well as newer liquid biopsy blood tests. Tumors often grow for months or years before causing noticeable symptoms, and modern screening methods can identify cancer at the cellular or molecular level. This pre-symptomatic detection can improve treatment options and, for many cancers, increase the chances of successful outcomes.
16. What is multi-cancer early detection testing?
Multi-cancer early detection (MCED) testing uses a single blood test to screen for signals associated with multiple cancer types, sometimes before symptoms appear. Depending on the test, this may involve analyzing DNA, proteins, or other biomarkers. Some MCDE tests can screen for 20 or more different cancer type. . PanTum Detect is an example of this innovative MCED technology that offers a high sensitive and specific screening through a simple blood draw.
17. How accurate are PanTum Detect and other liquid biopsy tests?
PanTum Detect and other liquid biopsy tests for cancer detection show varying accuracy depending on the specific technology and cancer types being screened. Current generation tests demonstrate high specificity (low false positives) with sensitivity that varies by cancer stage and type. These tests are most effective when used as part of a comprehensive screening strategy alongside traditional methods. Discover PanTum Detect accuracy data →
18. What cancers can PanTum Detect and liquid biopsy screen for?
Modern liquid biopsy tests including PanTum Detect can potentially detect multiple cancer types from a single blood sample, including cancers that lack established screening programs. PanTum Detect works by identifying immune responses to cancer rather than detecting tumor material directly, offering a unique approach to multi-cancer screening. View PanTum Detect cancer detection capabilities →
Medical Disclaimer
This article is for informational purposes only and should not be considered medical advice. Always consult with qualified healthcare professionals before making decisions about cancer screening, testing, or treatment. Individual health circumstances vary, and screening recommendations should be personalized based on your specific risk factors, medical history, and current health status.
References and Further Reading
For those interested in diving deeper into the research behind early cancer detection, we recommend exploring: